Phagocytes is the collective name for Macrophages and Dendritic cells. Phagocytes are large white cells that can engulf and digest foreign invaders.
Phagocytes generally patrol the body searching for pathogens, but can be called to specific locations by cytokines.
Only professional antigen-presenting cells, (macrophages, B lymphocytes, and dendritic cells) are able to activate a helper T-cell which has never encountered its antigen before.
Some immune cells have more than one name. For example:-
Phagocytes, refers to the large immune cells that can engulf and digest foreign invaders, and
Granulocytes, refers to immune cells that carry granules laden with killer chemicals.
Phagocytes include :-
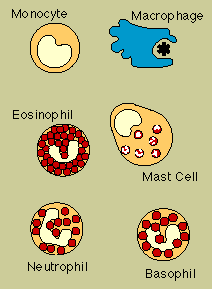
Monocytes, which circulate in the blood;
Macrophages, which are found in tissues throughout the body. Macrophages are versatile cells. Besides acting as phagocytic scavengers, they secrete a wide variety of signaling cytokines (called monokines) that are vital to the immune response.
Dendritic cells, which are more stationary, monitoring their environment from one spot such as the skin. Dendritic cells are the most potent of all the antigen-presenting cells.
Neutrophils, are in fact both a phagocyte and granulocyte cell that circulate in the blood but move into tissues when they are needed. They contain granules filled with potent chemicals. which in addition to destroying micro- organisms, play a key role in acute inflammatory reactions. Other myeloid descendants become granule-containing inflammatory cells known as Granulocytes.
Types of Granulocytes include:-
Eosinophils and Basophils, which degranulate by spraying their chemicals onto harmful cells or microbes.
The Mast cell is a twin of the basophil, except it is not a blood cell. Rather, it is responsible for allergy symptoms in the lungs, skin, and linings of the nose and intestinal tract.
A related structure, the blood platelet, is a cell fragment. Platelets, too, contain granules. They promote blood clotting and wound repair, and activate some immune defences.
http://users.rcn.com/jkimball.ma.ultranet/BiologyPages/E/Endocytosis.html
The Functions of these cells- fall into three categories,
1) Phagocytosis
2) Secretion of cytokines. Diverse and potent chemical messengers secreted by the cells of the immune system, and are the chief tool of T cells.
3) Antigen presentation.
Phagocytosis
These cells listed below, which arise from the bone marrow, have a variety of functions in the immune response:
The cells performing these various functions have differing microscopic appearances but they are grouped together as the Mononuclear Phagocytic System.
Phagocytosis is sometimes described as 'cell eating' but it is not really a process by which the cell obtains nourishment. White blood cells called neutrophils and other cells of the immune system carry out phagocytosis to keep the body clear of unwanted bacteria and parasites.
When the phagocytic white cell detects bacteria, it moves its cytoplasm and cell wall towards the bacteria, in a sort of creeping motion. The extensions of the cell that form during this movement are called pseudopodia meaning "false feet."
The cell membrane of the white cell completely surrounds a bacterium, enclosing it in a self contained vesicle called a phagosome. This vesicle is inside the white cell but the bacteria is a prisoner, surrounded by an internal cell wall to keep it away from the cell's cytoplasm. The cell then moves lysosomes, vesicles full of digestive enzymes, towards the phagosome and these discharge into the inside of the bacterium's vesicle, where they kill it and degrade it. The cell then spits the bits out.
The debris is moved towards the cell membrane and the membrane of the vesicle fuses with the cell membrane, pushing the debris out of the cell. Phagocytosis is the engulfment and digestion of bacteria and other antigens by phagocytes.
Monocytes
Monocytes are a type of agranulocyte, which are in turn a type of leucocyte (white blood cells). Agranulocytes (including monocytes) are distinguished from the other category of leucocytes because agranulocytes do not contain chemical-filled cytoplasmic vesicles called "granules".
An important function of monocytes is combatting microbes by the process of phagocytosis (after transforming into fixed or wandering macrophages).

When a monocyte enters damaged tissue through the endothelium of a blood vessel, (a process known as the leukocyte adhesion cascade) it undergoes a series of changes to become a Macrophage.
Monocytes are attracted to a damaged site by chemical substances through chemotaxis triggered by a range of stimuli including damaged cells, pathogens, histamine released by mast cells, basophils, and cytokines released by macrophages already at the site.
http://en.wikipedia.org/wiki/Monocyte
Macrophages
A large cell that is derived from a white blood cell called a monocyte, that ingests bacteria and other foreign cells, and that helps white blood cells identify microorganisms and other foreign substances.
Macrophages act as scavengers, they secrete a wide variety of powerful chemicals, and they play an essential role in activating T cells. Unlike short-lived neutrophils the life span of a macrophage ranges from months to years. Macrophages are cells within the tissues that originate from specific white blood cells called monocytes. Monocytes and macrophages are phagocytes acting in both non-specific defence (or innate immunity) as well as specific defence (or cell-mediated immunity) of vertebrate animals.
Their role is to phagocytose (engulf and then digest) cellular debris and pathogens either as stationary or mobile cells, and to stimulate lymphocytes and other immune cells to respond to the pathogen.
Macrophages cells reside within tissues and produce a wide array of chemicals including enzymes, complement proteins and regulatory factors, such as interleukin1.
Macrophages also act as scavengers, ridding the body of worn-out cells and other debris. Macrophages are also antigen presenting cells that activate the adaptive immune system.
http://en.wikipedia.org/wiki/Macrophage
Dendritic Cells
Dendritic cells (DC) are phagocytes in tissues that are in contact with the external environment, therefore, they are located mainly in the skin nose, lungs, stomach and intestines.
They are named for their resemblance to neuronal dendrites, as both have many spine-like projections, but dendritic cells are in no way connected to the nervous system.
Dendritic cells serve as a link between the innate and adaptive immune systems, as they present antigen to T cells; one of the key cell types of the adaptive immune system.
The principal function of dendritic cells is to act as the central command and central encyclopedia of the immune response, or similar to servers in a computer network.
They collect and store the immune system's "knowledge",enabling them to instruct and direct the adaptive arms in response to challenges.
Dendritic Cells process antigen material and present it on the surface to other cells of the immune system, thus functioning as Antigen-presenting cells. Dendritic cells are present in small quantities in tissues that are in contact with the external environment, mainly the skin, ( where they are often called Langerhans cells) and the inner lining of the nose, lungs, stomach, and intestines.They can also be found in an immature state in the blood. Once activated, they migrate to the lymphoid tissues where they interact with T cells and B cells to initiate and shape the adaptive immune response. At certain development stages they grow branched projections, the dendrites that give the cell its name. Immature dendritic cells are also called veiled cells, in which case they possess large cytoplasmic 'veils' rather than dendrites.
http://en.wikipedia.org/wiki/Dendritic_cell
Neutrophils
Neutrophils are fast acting, an "eater" (but do not survive after ingestion)
Neutrophils are not only phagocytes but also granulocytes. They contain granules filled with potent chemicals. These chemicals, in addition to destroying micro-organisms, play a key role in acute inflammatory reactions. Neutrophils, also known as polymorphonuclear leukocytes, are found in the tissues during acute inflammatory processes. Neutrophil Polymorph's are also involved in the effector side of the immune response. ( cells which mediate an immune response, or a molecule that binds to an enzyme with an effect on its catalytic activity, i.e. either an activator or inhibitor.)
They are the most common type of white blood cell ,known as Granulocytes which make up about 50-70% of all white blood cells. They are phagocytic, meaning that they can ingest other cells, though they do not survive the act.
Neutrophils are the first immune cells to arrive at a site of infection, through a process known as chemotaxis. (movement by a cell or organism in reaction to a chemical stimulus) In this response to chemotactic signals, they leave capillaries by a complex process, flowing nearer to the endothelial lining of blood vessels, rolling and then attaching. (margination)
They then emigrate between the endothelial cells (extravasation, or diapedesis), in which several mediators are involved.
These include substances produced by micro-organisms, and by the cells participating in the inflammatory process. One such, is a substance called interleukin-1 (IL-1), which is released by macrophages as a result of infection or tissue injury.
Another is histamine, released by circulating basophils, tissue mast cells, and blood platelets. It causes capillary and venular dilatation (small veins which connect capillaries to large veins).
The activation of Complement produces C3a and C5a which are chemotactic for phagocytic cells.(causing by chemical stimulation, in this case the Neutrophil to move along the pathway.see picture)
Chemotaxis  Another group of substances produced are the acute phase proteins. As a consequence of tissue damage, the liver produces a substance called C-reactive protein (CRP), which is so called on account of its ability to attach to the C-polysaccharide component of the cell wall of bacteria and fungi.
Another group of substances produced are the acute phase proteins. As a consequence of tissue damage, the liver produces a substance called C-reactive protein (CRP), which is so called on account of its ability to attach to the C-polysaccharide component of the cell wall of bacteria and fungi.
This activates the complement system by the classical pathway, and as a result C3a is formed and coats the organism, facilitating it's phagocytosis. (the process in which phagocytes engulf and digest micro-organisms and cellular debrisa defence against infection)
Though neutrophils are short lived, with a half life of four to ten hours when not activated, and immediate death upon ingesting a pathogen, (disease causing cell), they are plentiful and responsible for the bulk of an immune response.
They are the main component of pus and responsible for its whitish color.
Neutrophil Granulocytes are released from the bone marrow, by Regulatory Complement Proteins, (RCP's) and are present in the bloodstream until signaled to a site of infection by chemical cues in the body.
They are fast acting, arriving at the site of infection within an hour.
Other Types of Granulocytes are.... Eosinophils, Basophils. and Mast cells are granule-containing cells in tissue.
Eosinophils are so named because their cytoplasmic granules stain red with the dye eosin. They are also known as eosinophilic leukocytes.
Eosinophil granulocytes, usually called eosinophils (or, less commonly, acidophils), are white blood cells of the immune system that are responsible for combating infection and parasites in verterbrates. They also control mechanisms associated with allergy and asthma. They are granulocytes that develop in the bone marrow before migrating into blood.
Within their cellular cytoplasm are a diverse collection of chemical mediators, such as histamine, and proteins such as eosinophil peroxidase, RNase, DNases, lipase, plasminogen, and Major Basic Protein.These mediators are released by a process called degranulation, following activation of the eosinophil, and are toxic to both parasite and host tissues.
They are found in the medulla and the junction between the cortex and medulla of the thymus and, in the lower gastrointestinal tract, ovary, uterus, and spleen, and lymph nodes, but not in the lung, skin or oesophagus, or some other internal organs under normal conditions. The presence of eosinophils in these latter organs is associated with disease. Eosinophils persist in the circulation for 8-12 hours, and can survive in tissue for an additional 8-12 days in the absence of stimulation.
Basophils
Basophils are the least common of the granulocytes and contain large cytoplasmic granules. The Mast Cell, (see mast cells) a cell in tissues, has many similar characteristics. For example, both cell types store histamine, a chemical that is secreted by the cells when stimulated.
(histamine causes some of the symptoms of an allergic reaction).
Like all circulating granulocytes, basophils can be recruited out of the blood into a tissue when needed.
When activated, basophils degranulate to release histamine, proteoglycans,(eg:heparin and chondroitin) and proteolytic enzymes (eg: elastase and lysophospholipase). They also secrete lipid* (see definition below) mediators, like leukotrines, and several cytokines. Histamine and proteoglycans are pre-stored in the cell's granules while the other secreted substances are newly generated. Each of these substances contributes to inflammation. Recent evidence suggests that basophils are an important source of the cytokine, interleukin-4, perhaps more important than T cells. Interleukin-4 is considered one of the critical cytokines in the development of allergies and the production of IgE antibody by the immune system.
There are other substances that can activate basophils to secrete, which suggests that these cells have other roles in inflammation. A low basophil count (Basopenia ) is difficult to demonstrate as the normal basophil count is so low; it has been reported in association with autoimmune Urticaria (a chronic itching condition).
Definition of *lipid (Any of a group of organic compounds, including the fats, oils, waxes, sterols, and triglycerides, that are insoluble in water but soluble in nonpolar organic solvents, are oily to the touch, and together with carbohydrates and proteins constitute the principal structural material of living cells.)
Mast Cells
Mast cells reside in connective tissues and mucous membranes and regulate the inflammatory response. They are most often associated with allergy and anaphylaxis.
Basophils and eosinophils are related to neutrophils. They secrete chemical mediators that are involved in defending against parasites and play a role in allergic reactions, such as asthma. Natural killer cells (NK's), are leukocytes that attack and destroy tumor cells, or cells that have been infected by viruses
A mast cell (or mastocyte) is a resident cell of several types of tissues and contains many granules rich in histamine and heparin.
Although best known for their role in allergy and anaphylaxis, (hypersensitivity reaction to the ingestion or injection of a substance (a protein or drug) resulting from prior contact with a substance), mast cells play an important protective role as well, being intimately involved in wound healing and defence against pathogens. Mast cells are very similar to basophils in blood.
The similarities between mast cells and basophils has led many to speculate that mast cells are basophils that have "homed in" on tissues. However, current evidence suggests that they are generated by different precursor cells in the bone marrow. Both mast cells and basophils are thought to originate from bone marrow precursors expressing the CD34 molecule.
The basophil leaves the bone marrow already mature while the mast cell circulates in an immature form, only maturing once in a tissue site.
The tissue site an immature mast cell chooses to settle in, probably determines it's precise characteristics.
Two types of mast cells are recognized.
1) those from connective tissue
2)and a distinct set of mucosal mast cells.
The activities of the mucosal mast cells are dependent on T-cells. Mast cells are present in most tissues in the vicinity of blood vessels, and are especially prominent near the boundaries between the outside world and the internal milieu, such as the skin, mucosa of the lungs, and digestive tract, as well as in the mouth, conjunctiva and nose.
Mast cells are also involved in the effector side of the immune response. (cells which mediate an immune response, or a molecule that binds to an enzyme with an effect on its catalytic activity, i.e. either an activator or inhibitor) Recent evidence suggests that mast cells may be important mediators of regulatory t cell dependent peripheral (around the body) tolerance.
